The Perplexing Case of Darkening Skin: A Medication's Unseen Side Effect
Introduction
When a patient presents with unexpected symptoms, physicians often embark on a diagnostic journey that can be both challenging and enlightening. Such was the case for a woman who developed dramatic skin changes—turning black and blue—just weeks after starting a new medication. This case highlights the importance of considering adverse drug reactions when faced with unexplained clinical signs.
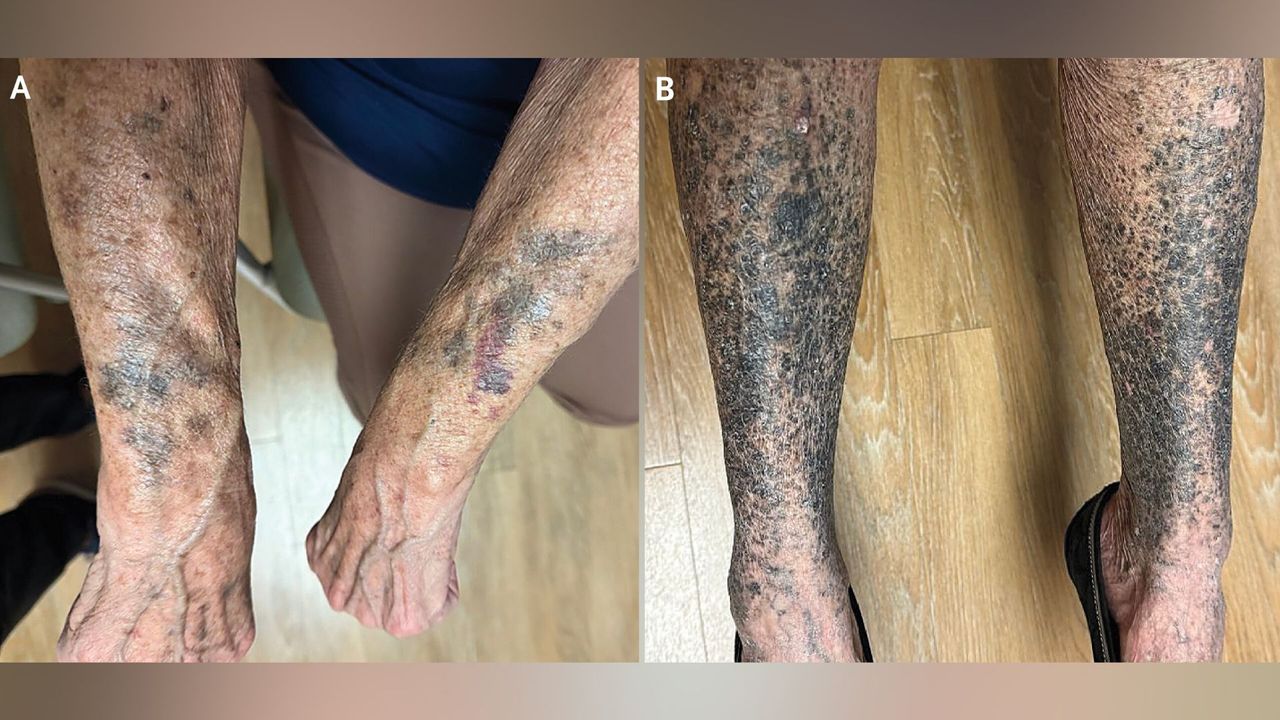
The Patient's Story
A middle-aged woman sought medical attention after noticing a gradual but striking darkening of her skin. The discoloration, described as a mix of black and blue patches, appeared primarily on sun-exposed areas but later spread to other parts of her body. She had been in good health prior to this episode, and the only recent change was the introduction of a new medication prescribed for a chronic condition. The timeline was suspicious: symptoms emerged roughly three weeks after she began the drug regimen.
Diagnostic Process
Initial Examinations
Doctors initially considered common causes of hyperpigmentation, such as hormonal imbalances, autoimmune disorders, or genetic conditions. Blood tests and skin biopsies were performed to rule out conditions like Addison's disease, hemochromatosis, and melanoma. However, all tests came back normal.
The Key Clue
It was the patient's medication history that provided the breakthrough. A review of her prescriptions revealed that one of the drugs was known to cause skin pigmentation in rare cases. The medical team consulted dermatologists and pharmacologists to confirm the association.
The Culprit: Medication Side Effect
The specific mechanism involves the drug or its metabolites accumulating in the skin, often binding to melanin or triggering an inflammatory response that leads to hyperpigmentation. In this case, the medication was a commonly prescribed antibiotic known to cause such effects in a small subset of patients. The discoloration was not a sign of an allergic reaction but rather a direct pharmacological side effect.
Risk Factors
- Prolonged use of the medication (weeks to months)
- High cumulative doses
- Sun exposure, which can exacerbate pigmentation
- Individual genetic susceptibility
Management and Outcome
Once the diagnosis was established, the immediate step was to discontinue the offending drug. In many cases, hyperpigmentation gradually fades over months to years after stopping the medication. The patient was advised to use strict sun protection to prevent further darkening and to monitor for any additional side effects. A follow-up plan was put in place to track the resolution of her skin discoloration.
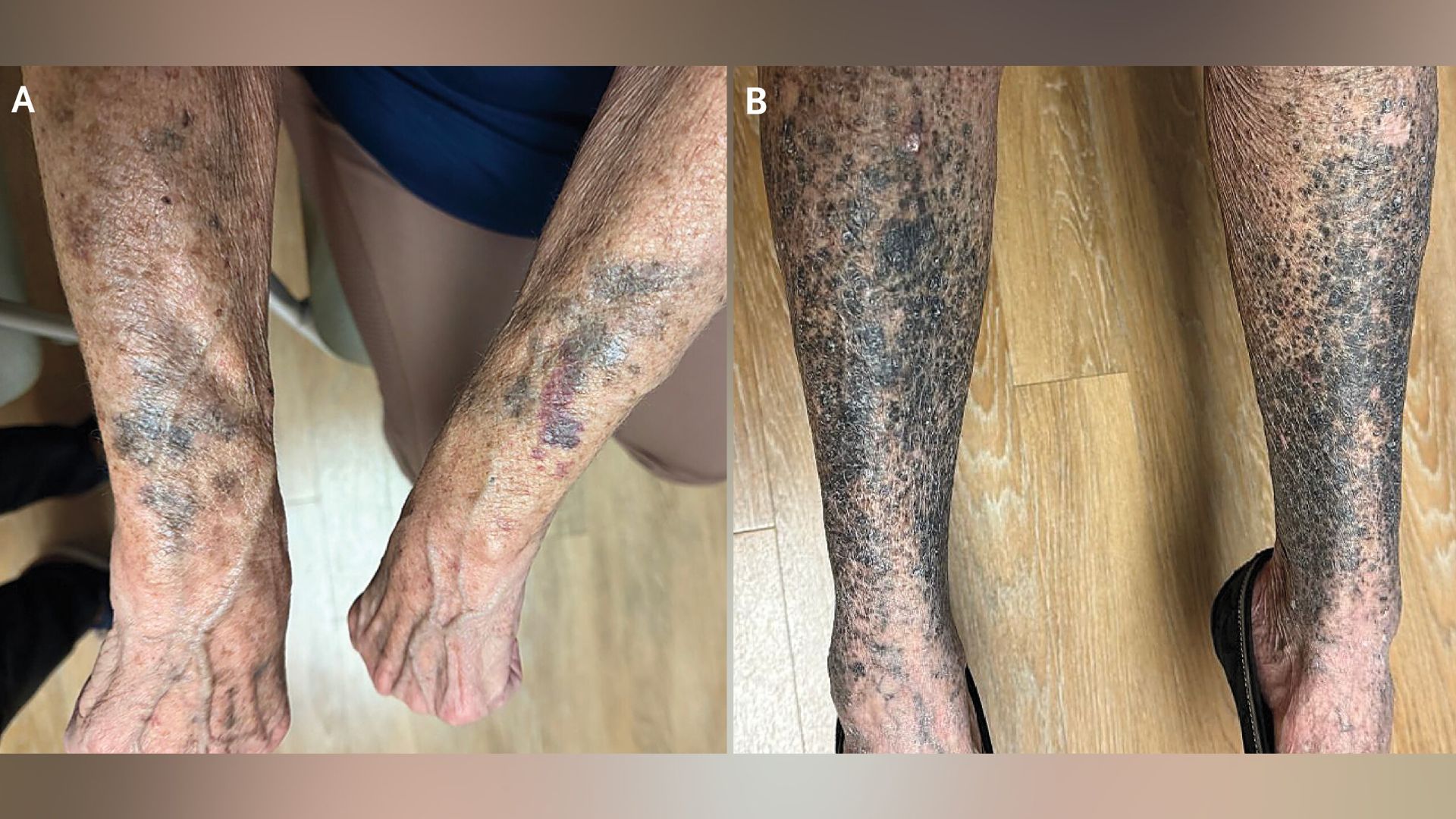
For some patients, switching to an alternative medication may be necessary. In this instance, the underlying condition was managed with a different class of drugs that did not carry the same risk. The patient’s skin slowly returned to its normal tone, though complete resolution took nearly a year.
Key Takeaways
This case serves as a reminder that medications can produce unexpected side effects beyond the well-known lists. Clinicians should maintain a high index of suspicion when patients present with unusual symptoms shortly after starting new drugs. The diagnostic dilemma often requires a multidisciplinary approach, including dermatology and pharmacology consultations.
For patients, it is crucial to report any new skin changes to their healthcare provider, especially if they coincide with the start of a new medication. Early recognition can prevent unnecessary tests and expedite resolution.
Conclusion
Sudden hyperpigmentation can be alarming, but in many instances, it is a reversible condition once the underlying cause is identified. The woman’s story underscores the value of thorough history-taking and the importance of considering drug-induced skin reactions in the broad differential of hyperpigmentation.
Back to Introduction | Read Patient Story | Diagnostic Process | Medication Side Effect Details | Key Takeaways
Related Articles
- Rising Global Threat: Dangerous Amoebas Spreading Due to Climate Change and Aging Infrastructure
- How to Reduce Your Baby's Exposure to PFAS in Formula
- How to Effectively Decontaminate Your Car Interior from Methamphetamine Residue
- Democrats Double Down on Affordable Health Care: Key Policy Questions Answered
- How to Trigger Your Brain's Natural Cleaning System with Simple Movements
- How to Reduce PFAS Exposure from Baby Formula: A Parent's Guide Based on FDA Findings
- Hinge Health's New FDA-Cleared Migraine Device: Everything You Need to Know
- 8 Key Milestones: Rivian's Revenue Surges as R2 Production Ramps Up